If you are planning to undergo knee replacement surgery, or if you have already had your knee replaced, this brochure is designed to support you in understanding how your rehabilitation can help you preparing for your surgery, as well as guide you in your recovery process so that you can return to an active, independent life as quickly as possible.
HOW CAN I IMPROVE MY PHYSICAL CONDITION PRIOR TO KNEE REPLACEMENT SURGERY?
Improving your physical condition prior to surgery is very important as it helps to ensure a more successful surgical procedure and recovery. To support you in ensuring that you are in the best shape possible, your surgeon will recommend that you do the following:
- Stop smoking and drinking alcohol;
- Stay active to keep your heart healthy;
- Exercise with your physiotherapist to improve your condition, muscle strength, and flexibility, reduce your pain, and help you learning how to walk with walking aids;
- Reduce weight if you are deemed overweight by seeking advice from your dietician and eating a well-balance diet.
BEFORE A KNEE REPLACEMENT SURGERY, WHAT ROLE DOES A PHYSIOTHERAPIST HAVE?
Prior to surgery, physiotherapists will support you in creating a tailored activity programme to suit your specific needs with safe and effective exercises or activities. Such programmes are designed to help soften your joints and leg muscles, increase your physical abilities as well as to learn the first post-operative exercises.
When practicing exercises, physiotherapists will work with you through every step. This will start slowly, beginning with a couple of minutes a few times a day, to then increase gradually to 20 or 30 minutes per day. Such exercises benefit heart, lungs, blood circulation and muscles, and are applied in a manner to ensure that you do not feel any pain. Examples include: walking on land or in water, cycling on stationary bike, or swimming.
Additionally, physiotherapists will advise you on how to use walking aids and the best ways to prepare your home to be a safe environment for when you return after your surgery.

WILL I NEED REHABILITATION AFTER KNEE REPLACEMENT SURGERY?
Yes, rehabilitation is an important part of a successful knee surgery procedure. Soon after the operation, physiotherapists will implement a programme to help you manage your pain effectively, recover your knee flexibility, reactivate your leg muscles, help you recover your gait and regain the ability to perform daily tasks again. This is all designed to help you return to your normal life as quickly as possible.
HOW DO I START REHABILITATION AFTER SURGERY?
After undergoing surgery, your surgeon will talk to you about starting daily inpatient rehabilitation with a physiotherapist. The first steps of a rehabilitation programme start on the day of the surgery and typically include:
- Establishing comfortable and safe positions;
- Controlling pain and swelling;
- Improving joint mobility and muscles strength;
- Learning how to change positions with assistance or by yourself;
- Learning how to stand and take first steps with a walking aid;
- Being educated on how to walk and climb stairs with walking aids, in preparation for returning home.

AFTER THE OPERATION, WOULD I NEED WALKING AIDS?
Based on each patient’s physical condition, your physiotherapist will provide safe and well-fitted walking aids, such as crutches or a walking frame to help you to walk safely and independently. You will then use these walking aids for several weeks until regaining a comfortable gait pattern.
DO I NEED TO PREPARE MY HOME FOR AFTER THE SURGERY?
Prior to hospitalisation, you will be advised to prepare your home to be a safe and comfortable post-surgical environment to return to. Examples of such changes include:
- Having your bedroom, bathroom and living room on the same floor. If this is not the case, you may want to place a bed on the same floor for this period;
- Hazards such as rugs, electrical cords etc. should be removed to avoid tripping;
- Ensuring the home has a high and firm seat chair with armrests;
- Install other specific equipment to make daily activities more comfortable, such as an elevated toilet seat, toilet safety rails, and a bathtub or shower bench.
As the rehabilitation progresses, you will be able to return to your normal daily life activities.
WHAT ARE THE BEST WAYS TO COPE WITH ANY PAIN THAT ARISES?
The key to managing pain is to always stay ahead of it. Therefore, prior to and after the surgery, physiotherapists will support you in controlling your pain through a wide range of medication-free techniques, such as:
- Cold therapy and cold compressive therapy programmes
- Leg positioning and exercising
- Active joint mobilisation
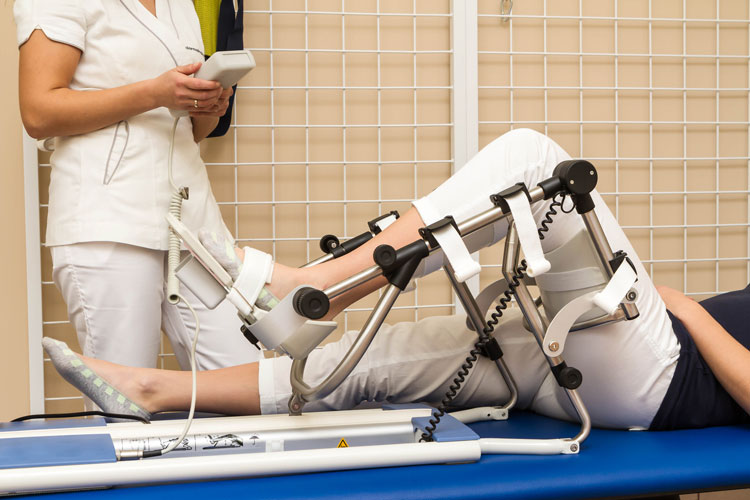
- Knee continuous passive motion device, which increases the mobility of joints
- Transcutaneous Electro Neuro Stimulation (TENS), which helps control pain.
WHAT STEPS CAN I TAKE TO SPEED UP MY RECOVERY?
Physiotherapists will look to guide you through each step of the rehabilitation process to help you recover as fast as possible. Actions which you can perform to support this include:
- Exercise as recommended by your physiotherapist, ensuring no over exertion;
- Control any pain prior and after exercise using cold packs for no more than 20 minutes, 4 to 6 times per day;
- Control leg swelling by elevating your leg;
- Re-position your knee frequently, alternating maximal flexion and full extension;
- Walk as recommended to avoid joint stiffness;
- Use compressive socks as advised by your doctor.
WHAT PRECAUTIONS SHOULD I TAKE AFTER KNEE REPLACEMENT SURGERY?
Generally, it is very important to follow all the instructions given by your surgeon and physiotherapist. Examples of such instructions are as follows:
- Do not put more weight on your operated leg than advised by your surgeon and physiotherapist;
- Keep your knee completely straight or completely bent. Do not keep your knee most of the time at a few degrees of flexion and lateral rotation;
- Do not twist your knee when turning your body. When sleeping on your good side, use a pillow under the affected leg;
- Do not cross your legs when sitting;
- Use stairs as instructed by your physiotherapist;
- Do not lift weights;
- Always use walking aids until your physiotherapist approves advancement. Do not stop using them except when otherwise recommended by your physiotherapist.
AM I PRONE TO FALLS AFTER KNEE SURGERY?
Yes, patients are more at risk of falling after surgery until they have completely recovered a normal gait. It is advised that you do not perform any activities such as getting out of bed and going up and down stairs alone unless recommended to do so. To limit the risk of falls, you should also:
- Use your walking aids as recommended
- Avoid wet floors;
- Wear rubber and well-fitted shoes;
- Ensure good lighting in the bathroom, corridor, bedroom etc;
- Change positions frequently to avoid joint stiffness;
- Ensure that a phone is always in easy reach;
- Ask for assistance if dizzy or tired;
- Follow instructions given by your physiotherapist.
WILL I NEED FURTHER REHABILITATION AFTER BEING DISCHARGED FROM HOSPITAL?
When you will be discharged from the hospital your surgeon will refer you to a physiotherapist to continue your rehabilitation programme as an outpatient. This programme will be adapted to your particular needs. It will normally take a few weeks before recovering pain-free mobility, functional flexibility and strength. Do not hesitate to talk with your physiotherapist to implement the best programme to fit your needs.

HOW LONG DOES THE OUTPATIENT REHABILITATION PROCESS NORMALLY TAKE?
Typically, most patients need four to six weeks to complete the rehabilitation programme, depending upon the type of work or activities they do or their level of fitness. For your specific case, you will be able to discuss this directly with your surgeon and physiotherapist to ensure the most suitable time and condition for you to return to work or regular activities.
Later on, you will be encouraged to participate in low-impact physical activities such as walking, swimming, cycling, tai-chi, golfing, aquatic gymnastics, table tennis, among others. High-impact physical activities though such as running, tennis, basketball, soccer, aerobics etc. are not recommended.
In addition, you will be advised not to drive your car or motorbike while taking pain medication or using crutches. Generally, patients are able to drive again four to six weeks following the operation. However, check with your surgeon before driving again. When you are deemed ok to drive yourself, you should then follow the driving precautions outlined by your physiotherapist.
WHEN SHOULD I CONTACT MY PHYSIOTHERAPIST?
At any point during or after the rehabilitation programme, you should contact your physiotherapist whenever you feel the need to. Typical reasons to do so include:
- Knee pain after exercising;
- Signs of swelling or knee becoming stiffer than usual;
- Being unable to practice exercise as recommended by your physiotherapist;
- Seeking advice on increasing an exercising programme;
- Needing additional advice on performing routine activities;
- Planning to start a new physical activity.
For more information, please contact:
PHYSIOTHERAPY & REHABILITATION DEPARTMENT
FV Hospital, 1st Floor, F Building
Tel (028) 54 11 33 40
Or (028) 54 11 33 33 – Ext: 1085 or 1485



