WHY BREASTFEED?
It’s best for your baby
Breast milk is the perfect food for your baby. No substitute comes close.
- Breast milk is filled with the vitamins and nutrients that your baby needs to grow and be healthy. It builds your baby’s immune system and helps his brain develop,
- Breast milk is easier to digest than formula – less vomiting and diarrhea,
- Breast milk changes as your baby grows, adjusting to his needs,
- Breastfed babies are less likely to have asthma, ear infections, allergies, and diabetes. They are also less likely to become obese,
- Breastfeeding reduces the risk of Sudden Infant Death Syndrome (SIDS).
It’s best for you
Being a new mom isn’t easy. Breastfeeding can help you make the transition.
- Breastfeeding helps your body recover from pregnancy and labor – shrinking your uterus back to size and reducing any bleeding after childbirth,
- It burns about 500 calories a day, so you lose more easily the weight which you have gained,
- It lowers the risk of ovarian cancer and some forms of breast cancer,
- It strengthens bones, protecting you against osteoporosis later,
- It may help ward off depression. It makes you feel relaxed and more confident,
- It saves time and money. Unlike formula, breast milk is always the right temperature, and requires no bottles to wash and sterilise.
It helps you feel close
Breastfeeding helps mothers and babies feel especially close.
Mom enjoys the special bonding time and the break that breastfeeding gives her during the busy early days. Baby is held close and cuddled, skin-to-skin, so he feels calmer and more secure.
HOW BREASTFEEDING WORKS
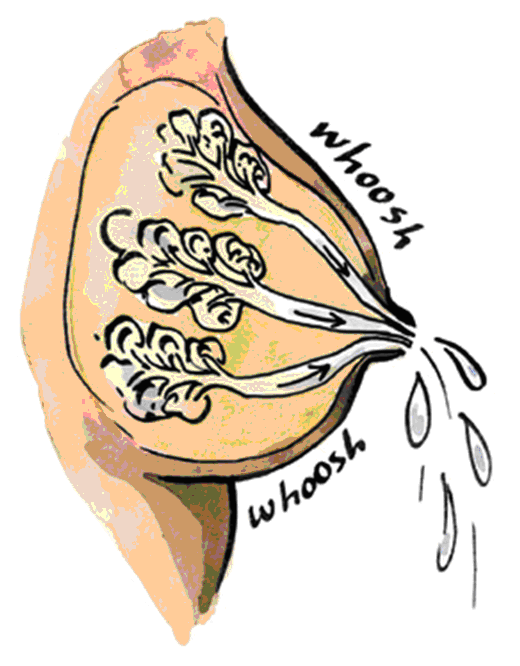
Breast milk is made in small sacs inside the breast. Muscles around the sacs squeeze the milk out. This is called the “let down”. Your let down works best when you are feeling comfortable and relaxed.
Colostrum is the thick and yellow milk made soon after your baby is born. It helps baby’s digestion and helps fight germs.
After a few days your milk looks thinner and paler. This is normal.
MYTHS – AND THE TRUTH

There are a lot of misconceptions about breastfeeding. Here’s the truth:
Myth: I won’t know if my baby is getting enough food.
Truth: It’s true there are no markers on your breast to measure quantities! But your baby will let you know when he/she is satisfied. In a 24-hour period, a well-fed baby will usually soil 3 diapers and wet at least 6 times.
Myth: Breastfeeding will make me fat.
Truth: Mothers who breastfeed usually lose their pregnancy weight faster than those who don’t.
Myth: Breastfeeding will ruin my breasts.
Truth: Breastfeeding doesn’t affect the shape of the breasts. Yes, your breasts lose their shape as you age. But you can slow the process by wearing a supportive bra, especially while you’re pregnant and breastfeeding.
Myth: My breasts are too small to make enough milk.
Truth: Any breast is the right size to breastfeed. A baby will eat as much as she needs and the more you breastfeed, the more milk you’ll make. To ensure your baby has enough milk to thrive, allow her to suck whenever she’s hungry.
Myth: Breastfeeding will make my baby’s other parent feel left out.
Truth: Breastfeed babies can be as close to their other parent as formula–fed babies are. There is a lot besides feeding that the other parent can do: make mom and baby comfortable when they’re feeding, change diapers, cuddle, burp, bathe, and play with the baby.
Myth: I won’t be able to breastfeed after I go back to work.
Truth: Many mothers breastfeed and work full time. Feed your baby right before you leave for work and right after you get home. If you can, express milk by hand or with a pump during the day and refrigerate it right away. Your caregiver can give it to your baby in a bottle. Expressed breast milk can be refrigerated for up to 3 days and frozen for 3 months. After thawing, use it within 24 hours.
Myth: I’ll have to go on a special diet to breastfeed.
Truth: You don’t have to do or eat anything special to breastfeed successfully. Even if your diet isn’t perfect, breast milk delivers the best nutrients. To feel your best, eat a healthy diet with at least 5 servings of fruits or vegetables every day, and drink plenty of water.
BREASTFEEDING YOUR BABY
Breastfeeding is natural for you and your baby, but it is a skill that needs to be learned. It may take little practice – for you and your baby. Speak up and ask questions about breastfeeding before your baby is born (during birth preparation sessions) and while you are in the hospital.
Getting Started
The first few days
- Breastfeed as soon as possible after birth,
- Ask that your baby be placed skin-to-skin on you as soon as your baby is born. Stay skin-to-skin until after the first breastfeeding. Being skin-to-skin helps babies cry less and stabilizes the baby’s temperature and breathing rate. It can also increase your milk supply,
- If you are cold, ask for a blanket to cover you and your baby. Your body heat will keep your baby warm as long as your baby’s back is covered. Your baby does not need to be tightly wrapped,
- If you have a Cesarean birth, you can still have skin-to-skin contact and breastfeed. You should be able to do this within the first three hours unless there is a medical reason not to,
- You can usually breastfeed if you have more than one baby. Your body will make enough milk to feed all your babies,
- Have your baby stay in your room. “Rooming in” encourages skin-to-skin contact and helps you recognize early feeding cues such as when your baby starts sucking his or her fist,
- Speak up and tell staff that you do not want your baby given formula or water, unless there is a medical reason for it. Ask staff not to give your baby a pacifier or bottle. These should not be given until your baby is about four weeks old, after breastfeeding is well established,
- Breastfeed before your baby is upset and crying,
- Breastfeed often. You’ll bond with your baby, he’ll learn to suck, and his sucking will build up your milk supply,
- It takes 3 to 5 days for your milk to come in. In the meantime, your body is making small amounts of a rich substance called Colostrum, which gives your baby everything he needs,
- It is important to know how to get the breastfeeding support you need in the hospital. You also need to know how you and your baby can stay healthy. These tips can help:

Ask your nurse to help you breastfeed. The nurse should watch you breastfeed several times before you leave the hospital. The nurse can tell if your baby is latching on and getting milk,
We do not recommend artificial nipples that may cause a decrease in milk supply. If you have trouble breastfeeding, ask your nurse for help,
Talk to your doctor or nurse about what you should eat or drink while you are breastfeeding.
Rooming-in
FV Hospital encourages rooming-in with your baby during your hospital stay. Rooming-in is good for both you and your baby. A mother who is rooming in is able to attend to her baby when feeding cues are displayed, helping her establish a good milk flow by promoting milk let-down. This means you are less likely to have hard, sore breasts and breastfeeding will get off to a good start. Rooming-in helps mothers bond with their babies and gain confidence in their care. Research shows that mothers and babies who room-in get more sleep.
The next few weeks
- Let your baby breastfeed whenever he/she wants, day and night. That will probably be every 2 to 3 hours – from 8 to 12 times in 24 hours. Frequent feeding will get your milk flowing and help your baby grow,
- By 4 to 5 weeks, your baby will probably have a more regular, less frequent, feeding pattern,
- Until you’ve established a good breast-feeding routine, avoid using a bottle.
Always
Wash your hands before you breastfeed your baby or express milk.
How long?
Any amount of breastfeeding is good for your baby – the longer, the better. Some mothers breastfeed for 12 to 18 months, others less. Experts recommend exclusive breastfeeding for the first 4 to 6 months (when solid foods are introduced).
GETTING COMFORTABLE: POPULAR POSITIONS
If possible, sit upright in a chair to feed your baby. Use a footstool for comfort. This is usually better than sitting up in bed. Bring the baby to the breast, not the breast to the baby. Hunching over while breastfeeding may cause back pain. Use pillows to support your back and the arm that holds the baby. A pillow on your lap can raise the baby to a comfortable height. Take your time. Rushing only causes stress for you and your baby.
Feel free to experiment with different positions:
The cross cradle hold Your baby is on his/her side, supported by your arm, with his/her stomach touching yours. This position makes it easy to breastfeed without other people noticing.
The football hold Your baby is tucked under your arm, in a half-sitting position, while you support him/her head and shoulders from underneath.This is a good position to use after a cesarean birth, for a mother with large breasts, or for a sleepy baby.
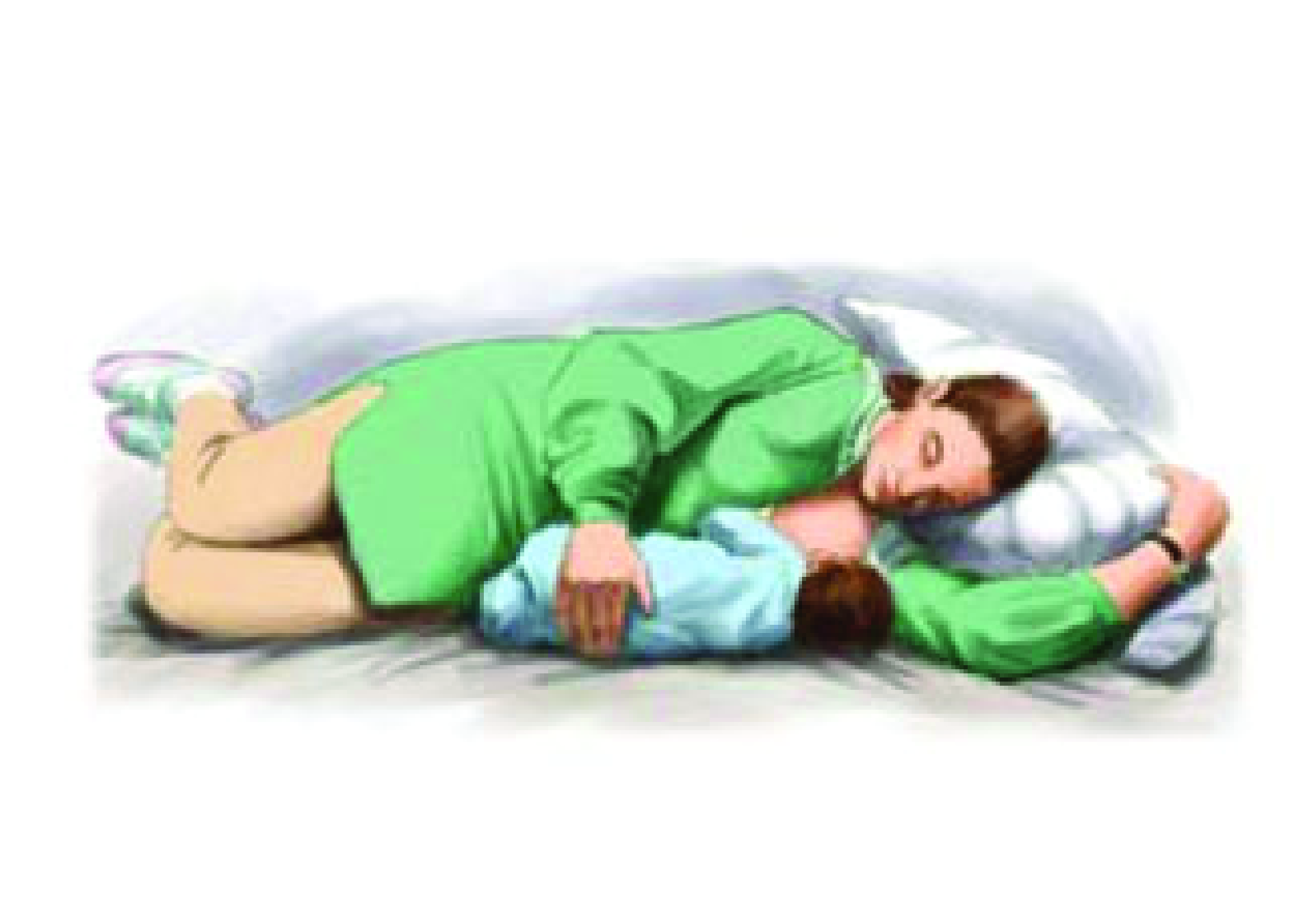
The side-lying position You and your baby are both on your sides, facing each other. This is a restful position for mother and baby, also good after cesarean birth.
“LATCHING ON” AND BREASTFEEDING
- Touch your baby’s cheek with your nipple. He/she will turn toward the side that you’ve touched. Once his/her head is in position, tickle your baby’s lips with the nipple Support your breast with your fingers underneath and your thumb on top. This is called the C-hold,
- When he/she opens his/her mouth wide, move it onto the nipple by pulling her toward you. This is called latching on. Apply a little pressure to his/her back. Get as much as possible of your aureola – the dark area around your nipple – into the baby’s mouth,
- If he/she has taken just the tip of the nipple, stick your clean pinky finger gently into the corner of his/her mouth to break the suction and tickle his/her lips with the nipple again until he/she opens wide,
- Breastfeeding shouldn’t hurt! Pain is a sign that your baby hasn’t latched on properly. If you feel pain, break the suction with your finger, take the baby off the nipple, and start over. Don’t let his/her breastfeed if he/she hasn’t latched on properly – it will encourage his/her to do it again in the future, and your nipples will become sore or cracked,
- Let your baby breastfeed whenever he/she is hungry and until he/she is satisfied – usually about 10 to 15 minutes on each breast. Some babies only take one breast at a feeding. Other babies take both breasts at each feeding. Help your baby finish the first breast, as long as he or she is still sucking and swallowing. This will ensure the baby gets the “hind” milk – the fattier milk at the end of a feeding. Offer the other breast if he or she seems to want more. Don’t worry if your baby breastfeeds for a shorter time on the second breast. Just start on that side next time. Your baby will let go of the breast when he or she is finished, and often falls asleep,
- When he/she pauses, burp him/her by putting him/her on your shoulder and patting or rubbing gently on his/her back.
BREASTFEEDING AND YOUR DIET

Now is not the time to diet! Breastfeeding helps you lose weight after your baby is born. Breastfeeding women should eat a well balanced nutritious diet. It is important not to skip meals, but to eat a generous amount of fruits and vegetables, whole and grain breads and cereals, calcium and protein rich foods. You may become hungrier when you are breastfeeding.
It is best to satisfy your hunger with nutritious foods. No one food has been proven to upset babies or cause wind. The best advice is to eat all foods in moderation, unless there is a family history of food allergies or intolerance. The natural variation in your diet will change the flavour of the breast milk for your baby, which may better prepare your baby for solids after six months of age.
Breastfeeding mothers need enough fluids to stay hydrated. Drink to satisfy your thirst. Increasing the amount of fluid you drink does little to increase your milk supply. A minimal intake of caffeine is recommended for breastfeeding mothers. The younger the baby is the longer it will take any caffeine to be metabolised by their body. Excessive caffeine intake may make your baby wakeful and fussy. Remember caffeine can be found in tea, coffee, soft drinks, energy drinks, some medications, herbal preparations, as well as foods containing coffee or chocolate. Contrary to popular opinion alcohol does not increase milk supply but rather decreases milk let down and milk supply.
Current research recommends minimal alcohol intake while breastfeeding, no more than one to two alcoholic drinks per week. It is also recommended to wait two to three hours after drinking alcohol before breastfeeding your baby.
SPECIAL SITUATIONS

A premature or sick baby
Breast milk provides special benefits to premature and sick babies, helping them grow and preventing many diseases. If your baby is not able to nurse, you can express and freeze your milk until he/she gets better or is ready to feed by mouth. The nurses in NICU and the midwife can help you get started as soon as possible.
Your own illness
During most illnesses, such as colds, flu, and other infections, breastfeeding gives the baby your antibodies to protect against infection, so it is important to continue to breastfeed. If you are worried that your illness might hurt your baby, talk with your doctor.
Medications
Some over-the-counter drugs and prescription medications (including some kinds of birth control pills) should not be used by breastfeeding mothers. You can safely breastfeed even while you are taking most medicines. Your doctor can answer any questions you have about what’s safe and what’s not.
OVERCOMING PROBLEMS
With a little patience and persistence, almost any problem can be solved. Here are a few problems – and solutions

Engorged breasts
You may have overfullness or swelling of the breasts when your milk is coming in during the first 3 to 5 days after birth. This is called engorgement, and it goes away once your body becomes better at producing milk and no longer needs to store as much in advance. In the meantime:
- Shower or apply warm (not hot), wet washcloths to your breasts before you feed and cold compresses afterward,
- If your baby is having a hard time latching on, gently massage the area to squeeze out some milk before you offer the breast to relieve discomfort and reduce swelling,
- Breastfeed often (every 2 to 4 hours), from the painful side first offering both breasts at each feeding.
Sore nipples
If your baby isn’t latching on properly your nipples may get sore in the beginning. It helps to:
- Make sure your baby is taking as much areola in her mouth as possible,
- Try breastfeeding more frequently for shorter periods,
- Nurse on the less sore side first,
- Coat your nipples with breast milk after feedings and let them air dry for 15 minutes.
Blocked milk duct
A painful area or lump in the breast may mean a blocked duct.
- Make sure your bra fits properly, and avoid sleeping positions that put pressure on your breasts,
- Breastfeed often, from the painful side first.
- Drink lots of fluids and get lots of rest,
- Shower and apply warm, wet compresses to the painful breast,
- Gently massage the area.
Breast infection
A lumpy, painful breast accompanied by flu-like symptoms, such as chills, aches, and fever, may be a breast infection.
- Follow the steps for a blocked milk duct (above),
- Continue breastfeeding,
- Check with your doctor right away. You may need medication.
Breastfeeding is natural for you and your baby, but it is a skill that needs to be learned. Speak up and ask questions about breastfeeding before your baby is born and while you are in the hospital. This will help you continue to breastfeed after you go home. This brochure provides information to help you breastfeed your baby. Remember, you should always talk to your doctor or nurse about any tips or advice given to you about your health.