Table of contents
Casts and splints support and protect injured bones and soft tissue. When you break a bone, your doctor will put the pieces back together in the right position. Casts and splints hold the bones in place while they heal. They also reduce pain, swelling, and muscle spasm. Casts and splints are also applied in cases of soft tissue injury, tendinitis etc.
In some cases, splints and casts are applied following surgery.
Splints or “half-casts” provide less support than casts. However, splints can be adjusted to accommodate swelling from injuries easier than enclosed casts. Your doctor will decide which type of support is best for you.
TYPES OF SPLINTS AND CASTS
Casts are custom-made. They must fit the shape of your injured limb correctly to provide the best support. Casts can be made of plaster or fiberglass (which is a plastic that can be shaped).
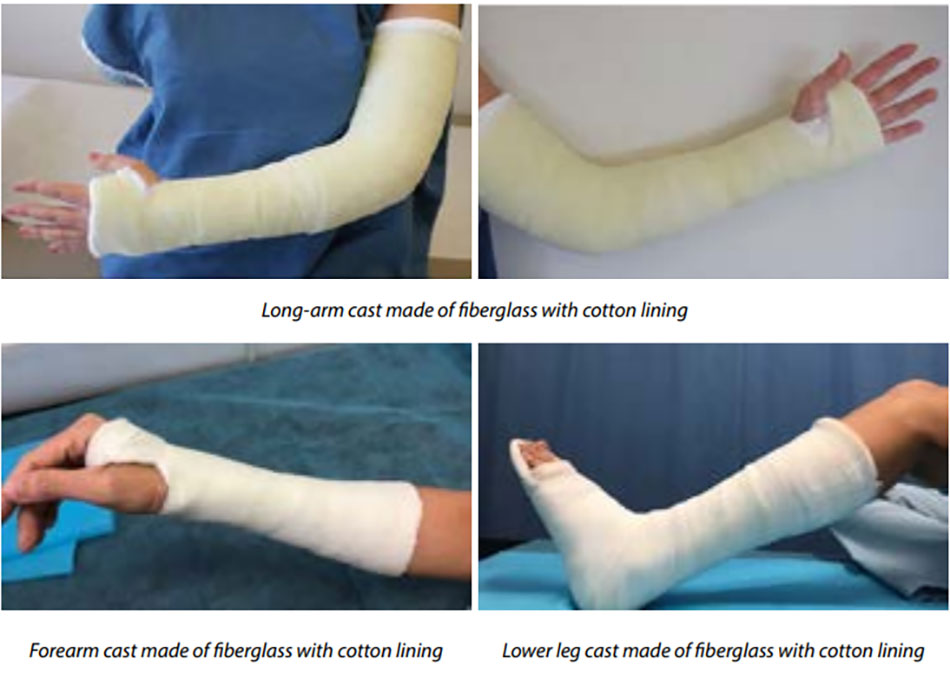
Splints or “half-casts” can also be custom-made, especially if an exact fit is necessary. Other times, a ready-made splint will be used. These off-the-shelf splints are made in a variety of shapes and sizes and are much easier and faster to use. Some have Velcro® straps which make the splints easy to put on, take off, and adjust.
To allow room for swelling, the rigid part of a splint or “half-cast” does not wrap all the way around the injured area. It is held in place with an elastic bandage or other material
Materials
Fiberglass or plaster materials form the hard, supportive layer in splints and casts. Fiberglass is lighter in weight and stronger than plaster. In addition, X-rays can “see through” fiberglass better than through plaster. This is important because your doctor will probably schedule additional X-rays after your splint or cast has been applied. X-rays can show whether the bones are healing well or have moved out of place.
Plaster is less expensive than fiberglass and shapes better than fiberglass for some uses.
Application
Both fiberglass and plaster splints and casts use padding, usually cotton, as a protective layer next to the skin. Both materials come in strips or rolls which are dipped in water and applied over the padding covering the injured area. In some cases, special waterproof padding and cast material may be used. Your doctor will let you know if your cast is made and padded with these waterproof materials.
The splint or cast must fit the shape of the injured arm or leg correctly to provide the best possible support. Generally, the splint or cast also covers the joint above and below the broken bone.
In many cases, a splint is applied to a fresh injury first. As swelling subsides, a full cast may replace the splint. If a cast is initially applied to your injury, it may be “valved” (cut) to allow for swelling, then repaired at your first follow-up appointment.
Sometimes, it may be necessary to replace a cast as swelling goes down and the cast gets “too big”. As a fracture heals, the cast may be replaced by a splint to make it easier to perform physiotherapy exercises.
GETTING USED TO A SPLINT OR CAST
Swelling due to your injury may cause pressure in your splint or cast for the first 48 to 72 hours. This may cause your injured arm or leg to feel snug or tight in the splint or cast. If you have a splint, your doctor will show you how to adjust it to accommodate the swelling.
It is very important to keep the swelling down. This will lessen pain and help your injury heal.
To help reduce swelling:
- Elevate: it is very important to elevate your injured arm or leg for the first 24 to 72 hours. Prop your injured arm or leg up above your heart by putting it on pillows or some other support. You will have to recline if the splint or cast is on your leg. Elevation allows clear fluid and blood to drain “downhill” to your heart;
- Exercise: move your uninjured, but swollen fingers or toes gently and often. Moving them often will prevent stiffness.
WARNING SIGNS
Swelling can create a lot of pressure under your cast or your splint. This can lead to severe problems.
COME IMMEDIATELY TO THE ACCIDENT & EMERGENCY DEPARTMENT if you experience any of the following symptoms:
- Increased pain and the feeling that the splint or cast is too tight
- Numbness and tingling in your hand or foot. This may be caused by too much pressure on the nerves
- Burning and stinging, feeling a rubbing or blister-like pain or discomfort within the cast. This may be caused by too much pressure on the skin that could lead to a pressure ulcer
- Excessive swelling below the cast. This may mean the cast is slowing your blood circulation
- Unpleasant smell or discharge coming from the cast
- Swelling, coldness, or blue-grey colour in the fingers or toes
- Numbness or loss of active movement of toes or fingers
- Shortness of breath and/or chest pain (in case of cast or splint on your leg)
TAKING CARE OF YOUR SPLINT OR CAST
Your doctor will explain any restrictions on using your injured arm or leg while it is healing. You must follow your doctor”s instructions carefully to make sure your bone heals properly. The following information provides general guidelines only and is not a substitute for your doctor”s advice.
After you have adjusted to your splint or cast for a few days, it is important to keep it in good condition. This will help your recovery.
Keep your splint or cast dry. Moisture weakens plaster and damp padding next to the skin can cause irritation. Use 2 layers of plastic or purchase waterproof shields to keep your splint or cast dry while you shower or bathe. Even if the cast is covered, do not submerge it or hold it under running water. A small pinhole in the cast cover can cause the injury to get soaked.
Walking casts. Do not walk on a “walking cast” until it is completely dry and hard. It takes about 1 hour for fiberglass, and 2 to 3 days for plaster to become hard enough to walk on. You will be given a cast shoe” to wear over your walking cast. The cast shoe will help protect the bottom of the cast.
Avoid dirt. Keep dirt, sand, and powder away from the inside of your splint or cast.
Padding. Do not pull out the padding from your splint or cast.
Itching. Do not stick objects such as coat hangers inside the splint or cast to scratch itching skin. Do not apply powders or deodorants to itching skin. If itching persists, contact your doctor. If something gets stuck inside your cast it may irritate your skin, so contact your doctor.
Trimming. Do not break off rough edges of the cast or trim the cast before asking your doctor.
Skin. Inspect the skin around the cast. If your skin becomes red or raw around the cast, contact your doctor.
Inspect the cast regularly. If it becomes cracked or develops soft spots, contact your doctor”s office.
Do not wear rings on fingers on your injured arm if you have a cast on it Use common sense. You have a serious injury and you must protect your cast from damage so it can protect your injury while it heals.
After the initial swelling has subsided, proper splint or cast support will usually allow you to continue your daily activities with a minimum of inconvenience.
CAST REMOVAL
Never remove the cast yourself. You may cut your skin or prevent proper healing of your injury.
Your doctor will use a cast saw to remove your cast. The saw vibrates, but does not rotate. If the blade of the saw touches the padding inside the hard shell of the cast, the padding will vibrate with the blade and will protect your skin. Cast saws make noise and may feel “hot” from friction, but will not harm you — “their bark is worse than their bite.” If you do feel pain while the cast is being removed, let your doctor or an assistant know and they will be able to make adjustments.
After the cast is removed, it is normal for there to be some discomfort in the bones and joints that were immobilised, for the arm or leg to be smaller than the other side, and for the skin to have some changes (dry skin and more hair).
A few baths in warm water will soak off the dry, flaky skin. This may take a few days, but be patient and avoid scrubbing the skin. You may apply some lotion to soften the skin, if desired. The hair will return to normal over several months.
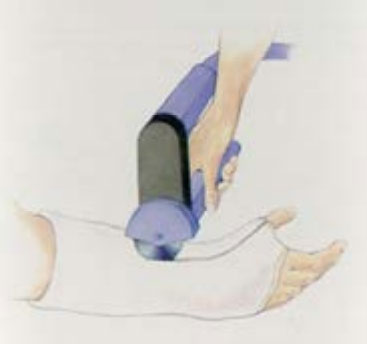
The saw vibrates but does not rotate.
Cast saws make noise but will not harm you.
REHABILITATION
While you are wearing your cast or splint, you will likely lose muscle strength in the injured area. Exercises during the healing process and after your cast is removed are important. They will help you restore normal muscle strength, joint motion, and flexibility.
CAN I TRAVEL ON A PLANE IF I HAVE A CAST?
It”s best to check with your travel operator or airline. Some airlines require you to wait 24 hours after a plaster cast has been fitted for flights less than 2 hours, and 48 hours for longer flights. This is because there”s a risk of swelling after a plaster cast is first fitted, which can affect your circulation.
If you”re planning to fly with a newly fitted plaster cast, you may need to have it split. This is done to prevent swelling and reduce the risk of deep vein thrombosis and compartment syndrome, a potentially serious condition caused by swelling.
If you have an upper body cast or your leg is in a plaster cast below your knee and you can bend your knee, you”ll be able to sit in a normal seat. If your plaster cast covers your knee, you won”t be able to bend it, so you”ll need to make special seating arrangements with your airline.
If you have a cast on your leg and need a wheelchair to get around the airport and board the plane, tell your airline as soon as possible. They can arrange for a wheelchair to meet you at both ends of your journey.



