What is Coumadin® and what is it used for?
Coumadin® (Warfarin) is a prescription medication used to treat blood clots and prevent the formation of clots in your body. Blood clots can block blood vessels and lead to critical conditions such as stroke, heart attack, or a vein blockage in the legs or lungs.
You might need to take warfarin because you have:
- Atrial fibrillation, an irregular heartbeat that can cause blood clots and stroke
- Blood clots in legs (deep vein thrombosis) or lungs (pulmonary embolism)
- Mechanical heart valves
Why are blood tests important?
The only way to check whether Coumadin® is working safely and effectively is by doing regular blood tests.
Coumadin® is monitored by a test called INR (International Normalized Ratio). It measures how thick or thin your blood is, and it is very important to determine and adjust the dosage of Coumadin®.
The INR goal is determined by your doctor, but is often ranged from 2 to 3. If the INR test comes back below the goal, it means that the blood is too thick. We are worried about you getting a clot, and probably need to increase your dose and vice versa.
When you first start taking Coumadin®, you will need to get your INR tested regularly for a few days, and then it will be tested periodically during your treatment with Coumadin® or in certain situations such as when you start or stop a medication that could change effect of Coumadin®, to ensure that your INR remains in the proper range.
What are the possible side effects of Coumadin®?
The most common side effect of Coumadin® is bleeding. Blood test is important to lower the risk of this side effect. An important note is that you might still bleed even if your blood test is within the range. Contact your doctor or go to the emergency room if something goes wrong.
Watch out for any signs or symptoms of bleeding such as:
- Pain, swelling, or discomfort
- Pink or brown urine
- Dark red or black stools
- Severe headache, dizziness or stomachache
- Unusual bruises that suddenly appear and grow in size
- Bleeding from cuts that take a long time to stop
- Uncontrollable nosebleed or bleeding gums
- Menstrual or vaginal bleeding that is heavier than usual
- Coughing up or vomiting blood; or vomiting material that look like coffee grounds
Rare side effects:
Serious, but rare side effects of Coumadin® include death of skin tissue or “skin necrosis” and “purple toe syndrome.” Notify your doctor right away if you see abnormal changes on any areas throughout your body.
How do I store Coumadin®?
Store Coumadin® at room temperature, in a cool and dry place. Do not store in the bathroom. Protect from light. Keep all drugs out of the reach of children and pets. Check with your pharmacist about how to throw out unused drugs.
What drugs interact with Coumadin®?
Coumadin® can change the way other medications work. At the same time, many other medications can affect the way Coumadin® works.
It is very important to let your doctor know that you are on Coumadin® before starting any medications (including herbals, natural and over-the-counter products).
- Some over-the-counter pain relievers can increase the risk of bleeding, including aspirin and anti-inflammatory drugs such as ibuprofen, diclofenac etc.
- Paracetamol is a safe choice for treating pain in patients on Coumadin®. However, if you need to take Paracetamol regularly (more than 3-4 times /week), let your doctor know as Coumadin® dose might need to be decreased.
- Some medications for the stomach can increase the effect of Coumadin®, including ranitidine, and bismuth subsalicylate.
- Many herbal medications can increase the effect of Coumadin®. This includes but not limited to garlic, ginger, gingko, ginseng, cranberry, feverfew, etc. Others can lower the effect of Coumadin®, such as St. John’s Worth or coenzyme Q10.
- Some antibiotics can also increase the effect and/or toxicity of Coumadin®.

Note: This is not a complete list of medicines or herbals that can affect Coumadin®. Consult your doctor whenever you need to start on any new medications.
Do I have to change my diet while on Coumadin®?
Food that contains high amount of vitamin K can interfere with the effectiveness of Coumadin® (reduces the effects of Coumadin® and increases the risk of clotting). Being CONSISTENT with your diet is necessary while taking Coumadin®. Talk to your doctor before making any diet changes.
Foods with high amount of vitamin K:
- Green leafy vegetables: Broccoli, Brussels sprouts, cabbage, collard greens, kales, lettuce, spinach, etc.
Foods with low amount of vitamin K:
- Fruits: apple, banana, blueberry, grape, orange, peach etc.
- Vegetables: carrot, cauliflower, eggplant, mushroom, potato, tomato etc.
- Beverage: coffee, milk, black tea etc.
Limit alcohol consumption

Is Coumadin® safe during pregnancy and breastfeeding?
Do not take Coumadin if you are pregnant or plan to become pregnant, Coumadin® can cause death or birth defects to an unborn baby. Use effective birth control methods if you are capable of becoming pregnant. Consult your doctor if you want to breastfeed while taking Coumadin®.
WHAT IS THE MOST IMPORTANT INFORMATION I SHOULD KNOW ABOUT COUMADIN™?
- Coumadin® helps to prevent blood clots.
- Make sure you know what tablets you are meant to be taking to make up your dose. Some people might need to take different doses every second days or on different days of the week.
- Take Coumadin® by mouth at the same time every day as directed by your doctor. Most people take their daily dose in the evening. This allows the dose to be changed if necessary on the next day that INR is obtained rather than waiting until the next day.
- If you miss a dose within 2-3 hours of your normal taking time, try to take it as soon as possible on that same day. Do NOT take a double dose of Coumadin® the next day to make up for the missed dose. A missed does may affect your INR blood tests. Make sure to document your missed dose so your doctor does not make unnecessary dose changes.
- Do NOT stop taking or change the dose of Coumadin® without talking to your doctor.
- Perform regular blood tests to check for your response to Coumadin® to avoid complications.
- Watch out for any signs and symptoms of bleeding and get help immediately.
- Inform your doctor and pharmacist about all your drug allergies and current medications, including herbals/supplements and over-the-counter products as Coumadin® can interact with many medications. Do NOT take Coumadin® if you are allergic to warfarin or any other ingredients in Coumadin®.
- Other medications can affect how well Coumadin® works. Always talk to your doctor or pharmacist before starting or stopping any medications including prescription or over-the-counter products, herbal supplements, vitamins or health supplements.
- Eat a normal, balanced diet with a consistent intake of green leafy vegetables. Some foods may interact with Coumadin® and affect your treatment. Do not make drastic changes in your dietary habits without consulting your doctor. Avoid drinking alcohol.
- Notify your doctor or go to emergency department if you notice any signs or symptoms of bleeding.
- Notify your doctor immediately if you take too much Coumadin®, are sick with diarrhea, an infection, or have a fever. If you fall, or get in an accident and hit your head, go to the hospital right away to get yourself checked.
- Always tell your healthcare providers (including dentists) that you are taking Coumadin®.
- Store Coumadin® in a cool, dry place.
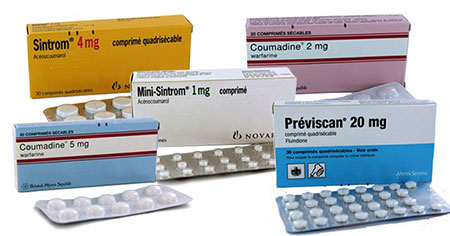
Other anti – vitamin K drugs:
This guide can also be applied to other anticoagulant drugs from the same class as warfarin (the class of anti-vitamin K medicines) such as:
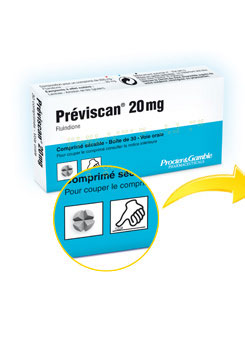
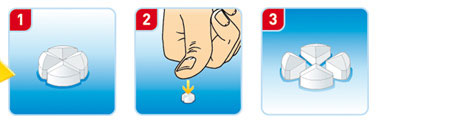
Fluindione (Previscan®)
Each tablet of 20 mg can be split easily into 4 quarters of 5 mg.
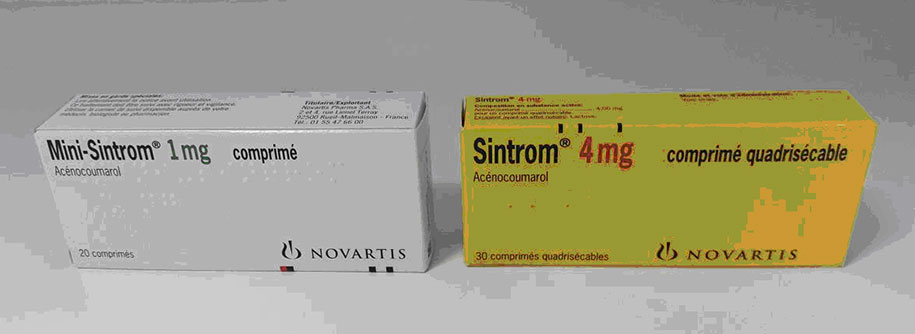
Acenocoumarol:
- Sintrom® 4 mg
- Mini-sintrom® 1 mg
These 2 dosages allow easy adjustment of the dose without the necessity to break the tablet into quarters.
Please contact your pharmacist for more information on these medications.



