Table of contents
After arriving at FV Hospital’s emergency room with severe abdominal pain and experiencing difficulty breathing, Johan Prasetyo Santoso, an Indonesian tourist, was shocked to hear from doctors that a large section of his stomach and intestines had moved to the chest cavity, causing compression of the heart and lungs, posing risk of death if he did not undergo surgery quickly.
A rare case of “straying stomach” – organs move from the abdomen to the chest
FV Hospital recently treated a rare emergency case. Johan Prasetyo Santoso, a 48-year-old male patient from Indonesia, arrived at FVH in critical condition. He was admitted to the hospital with severe abdominal pain, severe hiccups that had started three hours previously, and difficulty breathing. Mr Santoso was drenched in sweat and under extreme stress. The results of an abdominal CT scan showed that he had an acute diaphragmatic hernia and his stomach had migrated to his chest cavity.

Dr Tuan explains that the situation of a stomach moving into the chest cavity is very rare
The diaphragm is a flattened striated muscle which separates the thoracic cavity and the abdominal cavity. In addition to its main function to support respiration, the diaphragm also acts as a partition to separate organs in the chest and abdomen. A diaphragmatic hernia occurs when one or more abdominal organs move upward into the chest area through a defect or lesion on the diaphragm surface.
“When abdominal organs enter the ribcage and compress the heart and lungs, affecting breathing, emergency surgery is required to save the patient’s life. If this intervention is delayed, the organs can become stuck in the chest, causing inflammation, necrosis or rupture, leading to even greater risk of death,” says Dr Le Duc Tuan, a senior consultant at the General Surgery Department, FV Hospital.
Reviewing Mr Santoso’s medical history, Dr Tuan learned that the patient had been in a traffic accident six months prior. His ribs had been broken and Mr Santoso began to experience bouts of chest tightness and difficulty breathing afterwards. Mr Santoso visited his doctor many times in Indonesia, but was diagnosed with gastroesophageal reflux or a digestive disorder. No further examination, such as computerised tomography (CT) or magnetic resonance imaging (MRI), was performed.
“It is possible that the accident caused the patient’s diaphragm to rupture. When the patient eats too much or exercises vigorously, the underlying organs such as the stomach, intestines and greater omentum move upward, causing a diaphragmatic hernia. According to the world’s medical literature, only 0.3% of diaphragmatic trauma cases lead to a diaphragmatic hernia,” shares Dr Tuan.
Multi-specialty coordination is required to execute this complex surgery to return the stomach to the abdomen.
Dr Tuan adds that it was fortunate that Mr Santoso was brought to the hospital early. The patient’s ascending bowel was obstructed, but luckily was not yet necrotic. In case of necrosis or, more dangerously, bowel rupture, surgery must always be performed immediately. However, even this urgent intervention has a very high risk of death.
During examination, FV Hospital doctors found that nearly 30 centimetres of the stomach, intestines and greater omentum had passed through a hole in the diaphragm measuring five to six centimetres in diameter, forming a tight knot, making it difficult for the organs to be moved back. If maneuvered improperly, the intestines or stomach might rupture, or the surrounding vital organs might be traumatised. In addition, the patient’s heart was compressed on the side closest to the diaphragm hole, leading to the risk of cardiac arrest if surgical instruments came into contact with the heart while it continued beating. Another important issue for doctors is to control bleeding during surgery as it can prevent them from clearly seeing the organs, making it impossible to operate.
Mr Santoso’s laparoscopic surgery was anticipated to take eight hours, and involved a large team encompassing doctors from FV’s thoracic, digestive, vascular and imaging departments, led by Dr Tuan.
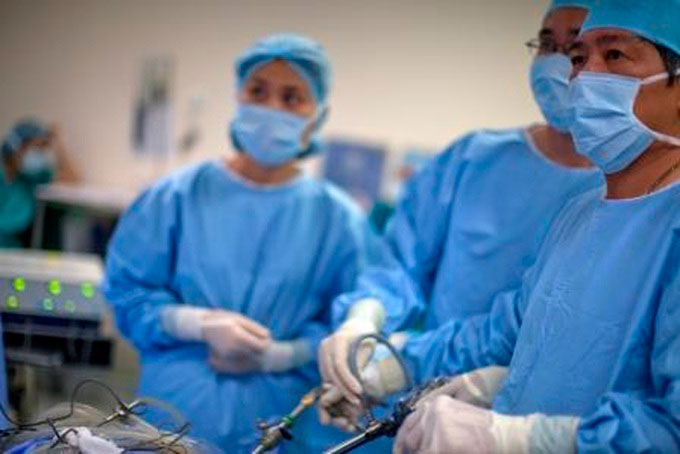
FV Hospital coordinates many specialties in surgery for Indonesian patient Mr Santoso
Despite careful planning, the doctors could not help but feel concerned. “This is a rare, complicated operation—the first time one nurse has witnessed an abdominal operation while both lungs and heart continue to function. For the first two hours, we moved the patient into different positions before finding a way to bring the intestines and stomach down to the abdomen without causing any further damage. The team was incredibly focused and worked in almost absolute silence,” says Dr Tuan.
The stomach and intestines were deflated to reduce their size. Dr Tuan used medical clamps to carefully pull down each organ, centimetre by centimetre, while blocking other organs from moving upwards. After more than four hours of stressful surgery, FV doctors had finally restored the herniated organs to the patient’s abdomen. However, as the severely compressed lung had collapsed, doctors had to place a pleural drain to help the lung expand.
“As soon as the bleeding stopped, the patient’s pulse, blood pressure and oxygen level on the monitoring screen returned to normal immediately. Initially, we prepared a room in the intensive care unit (ICU) to receive Mr Santoso after his surgery. However, we decided to send him to recovery because his condition was very good,” recalls Dr Tuan, adding that in this case, an open surgery may have been easier for the medical team to perform.
However, doctors would have had to make an incision that extends from the abdomen to the diaphragm, opening most of the abdomen. In that case, the patient would take longer to recover and would be classified as Health Level 4. FV doctors confidently chose laparoscopic surgery to ensure Mr Santoso would have a better quality of life immediately after the operation.
At 6 a.m. the next morning, Dr Tuan visited Mr Santoso in his room. He was welcomed by the bright smile of a patient who had been brought back from the brink of death, and had already regained his ability to move and was able to eat the same day.

Mr Johan Prasetyo Santoso and his wife thank Dr Tuan for helping him through the crisis
Returning to FV for a follow-up screening on December 12, Mr Santoso shared that he was extremely stressed when doctors first explained his CT scan results to him. “When Dr Tuan shared my situation, I was very scared, and I was far from my family. I called my doctor in Indonesia and after talking with FV doctors, they advised me to stay in Vietnam for treatment,” recalled Mr Santoso.
His condition meant that he could not delay the surgery and would be at increased risk of a bowel rupture if he chose to fly back home. However, when Dr Tuan advised him of the surgery plan and the modern medical equipment the team would use, Mr Santoso decided to trust FV doctors with his life.
“Talking with Dr Tuan, seeing that he is a very good doctor and is devoted to his patients, I felt completely assured. Now, I feel very well, and my wife and children are here by my side. My sincere thanks to Dr Tuan and his team for saving my life,” says Mr Santoso.
Please contact the General Surgery Department of FV Hospital via phone to book an appointment: (028) 35 11 33 33.



