Patient N.L., a 58-year-old woman from Cambodia, sought treatment at FV Hospital after six months of high-dose antifungal therapy in both Cambodia and Thailand failed to resolve her recurring haemoptysis. Dr Luong Ngoc Trung, MSc, Specialist Level II performed a successful robotic-assisted surgery using the da Vinci Xi system, preventing a potentially fatal outcome. Following the procedure, the patient made a remarkably swift recovery and was discharged within 3 days.
Six months of unsuccessful treatment and the looming threat of massive haemoptysis
N.L., a Cambodian national, was diagnosed with a lesion in the upper lobe of her left lung, confirmed as a pulmonary aspergilloma (fungal ball). Over 6 months, she received maximum-dose antifungal therapy at major hospitals in Cambodia and Thailand. Despite this, the lesion did not regress, and she continued to experience recurrent haemoptysis.
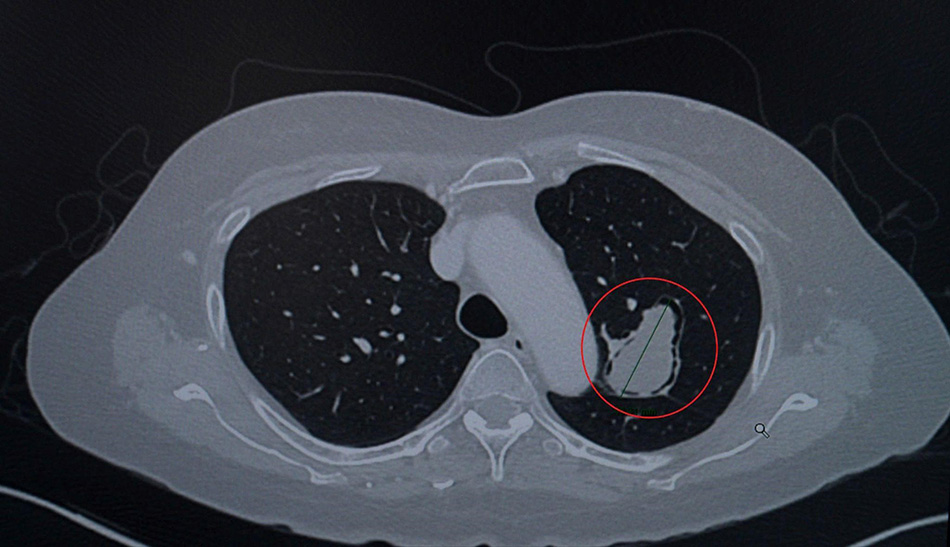
CT chest imaging showing the pulmonary aspergilloma (circled in red) in the upper lobe of the left lung, adjacent to the airway and thoracic aorta, measuring over 4cm in diameter. (Photo:FV)
She subsequently travelled to Vietnam to seek care at FV Hospital. Dr Luong Ngoc Trung, MSc, Specialist Level II – Head of Vascular & Endovascular Surgery Department, described her condition as a “ticking time bomb”. The aspergilloma measured up to 4.6 cm and was situated near the airway and thoracic aorta, posing a significant risk of vascular invasion or rupture.
This proximity created a danger of massive haemoptysis, a condition where blood floods the airway, which can lead to sudden death.
Furthermore, prolonged corticosteroid use had resulted in corticosteroid-induced Cushing’s syndrome and steroid-induced myopathy. The long-term antifungal regimen had also taken a significant toll on her health, leading to hepatotoxicity, nephrotoxicity, and a general physical decline.
Robotic-assisted surgery: An optimal approach for complex intrathoracic lesions
Given the urgency, the FV Hospital surgical team determined that pulmonary lobectomy, or complete removal of the affected lobe, was necessary to eliminate the infection. Instead of conventional thoracoscopic surgery, they chose the da Vinci Xi robotic system to ensure maximum precision.
Dr Luong Ngoc Trung, MSc, Specialist Level II explained that robotic-assisted surgery offers significant advantages in complex cases. “The robotic system allows precise, gentle manipulation even in the deepest recesses of the thoracic cavity, including areas near major hilar vessels, neurological structures, the pulmonary apex, and the spaces between the lung and heart. Surgical challenges in these locations can therefore be addressed with far greater accuracy and safety,” he said.
He added that the slender robotic arms, which can navigate confined anatomical spaces, reduce surgical invasiveness and minimise post-operative pain.
In this case, the robotic approach allowed controlled and meticulous removal of inflammatory pleural adhesions caused by chronic infection, while minimising the risk of intraoperative rupture of the aspergilloma. Rupture during dissection could result in widespread intrathoracic fungal contamination.
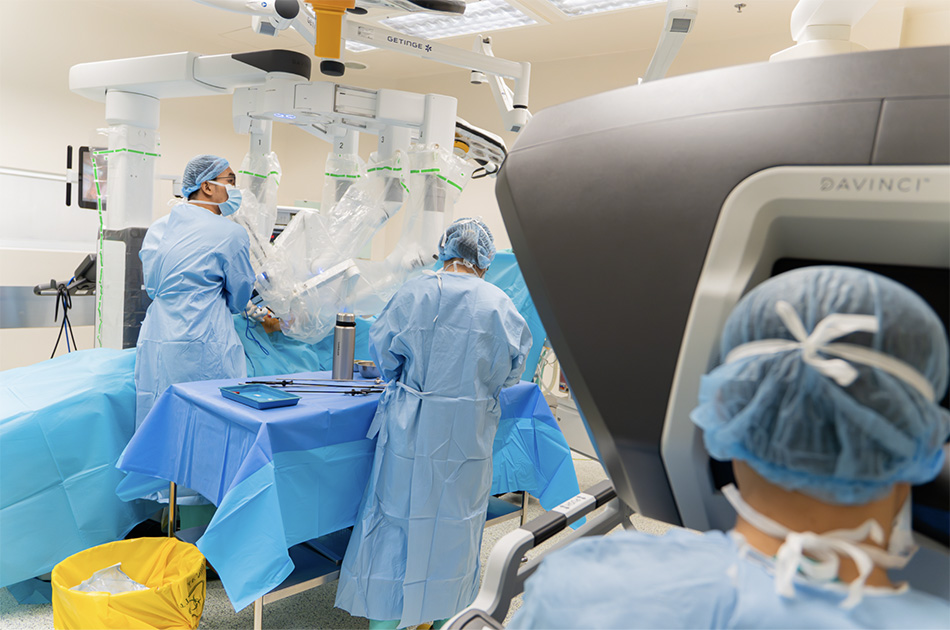
The FV Hospital surgical team performing robotic-assisted lobectomy, achieving complete resection of the complex pulmonary aspergilloma. (Photo: FV)
The procedure lasted about 140 minutes and focused on complete resection of the affected pulmonary lobe to eliminate the infection. The patient recovered quickly and was discharged 3 days after surgery.
At the most recent follow-up, her recovery was progressing well. She was able to discontinue antifungal therapy after a prolonged course. She continues to receive specialist care for corticosteroid-induced Cushing’s syndrome and myopathy from an endocrinologist.
Warning: Pulmonary Aspergilloma – the “silent killer”
Pulmonary aspergilloma can cause serious complications, most notably sudden, life-threatening haemoptysis. Clinicians advise patients with persistent cough, haemoptysis, or lack of response to antifungal therapy to seek specialist evaluation promptly. Timely integration of medical and surgical management is crucial for optimal outcomes and long-term prognosis.
Dr Luong Ngoc Trung, MSc, Specialist Level II emphasises that antifungal therapy remains the mandatory first-line treatment in pulmonary aspergilloma, even in patients for whom surgery is ultimately indicated.
However, if there is no response after active medical management, especially when the lesion is large and near critical structures, surgery is required for definitive cure.
In these cases, robotic-assisted surgery improves precision and safety, shortens recovery time, and reduces hospital stay and costs.
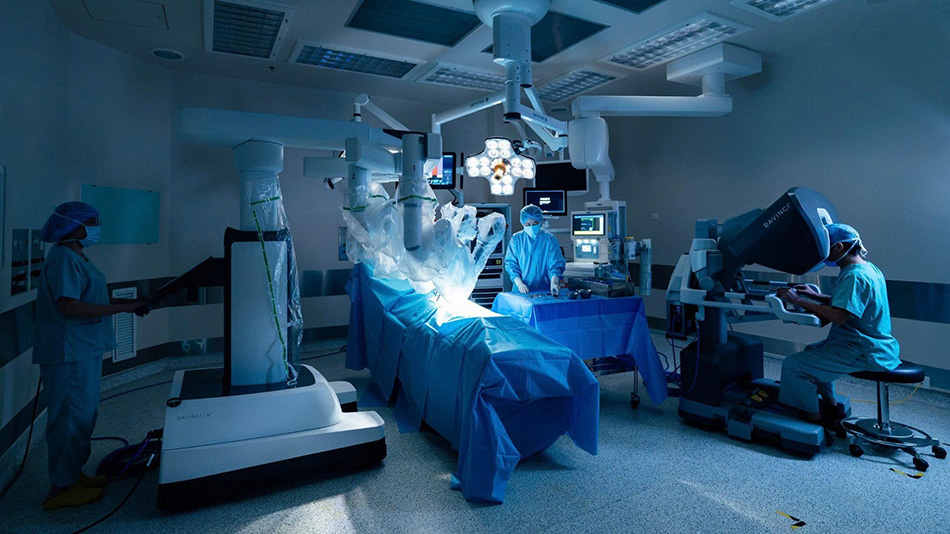
The da Vinci Xi robotic surgical system in use during the pulmonary aspergilloma procedure at FV Hospital, enhancing precision in deep intrathoracic dissection. (Photo:FV)
Robotic-assisted surgery is now used across multiple specialties at FV Hospital, including General Surgery, Urology, Thoracic Surgery, Gynaecology, and Oncology, with further expansion planned. This approach improves clinical outcomes and reduces patient invasiveness. FV Hospital employs highly experienced surgeons who have completed rigorous robotic surgery training and hold recognised certifications. All robotic procedures are performed in operating theatres that strictly follow JCI international healthcare standards, ensuring a sterile environment and minimising the risk of infection and complications.
To make this technology more accessible, FV Hospital is offering a VND40 million discount on selected da Vinci Xi robotic surgical procedures for the first 50 eligible patients, valid until June 15, 2026.
For more information, please visit FV Hospital at 6 Nguyen Luong Bang Street, Tan My Ward (formerly District 7), Ho Chi Minh City, or call (028) 3511 3333.



