Breast cancer is a very frequent cancer worldwide. In Vietnam its incidence has been increasing steadily and it is now the most common cancer affecting women.
What are the Symptoms of Breast Cancer?
Signs and symptoms of breast cancer may include:
- Change in the size, shape or appearance of a breast
- Changes to the skin over the breast, such as dimpling
- A newly inverted nipple
- Peeling, scaling or flaking of the pigmented area of skin surrounding the nipple (areola) or breast skin
- Redness or pitting of the skin over your breast, like the skin of an orange
When to see a doctor?
If you find a lump or other change in your breast — even if a recent mammogram was normal — make an appointment with your doctor for prompt evaluation.
What is the Cause of Breast Cancer?
It’s not clear what causes breast cancer.Doctors know that breast cancer occurs when some breast cells begin growing abnormally. These cells divide more rapidly than healthy cells do and continue to accumulate, forming a lump or mass. The cells may spread (metastasize) through your breast to your lymph nodes or to other parts of your body.
Breast cancer most often begins with cells in the milk-producing ducts (invasive ductal carcinoma). Breast cancer may also begin in the glandular tissue called lobules (invasive lobular carcinoma) or in other cells or tissue within the breast.
Researchers have identified hormonal, lifestyle and environmental factors that may increase your risk of breast cancer. But it’s not clear why some people who have no risk factors develop cancer, yet other people with risk factors never do. It’s likely that breast cancer is caused by a complex interaction of your genetic makeup and your environment.
What are the risk factors for breast cancer?
A breast cancer risk factor is anything that makes it more likely you’ll get breast cancer. But having one or even several breast cancer risk factors doesn’t necessarily mean you’ll develop breast cancer. Many women who develop breast cancer have no known risk factors other than simply being women. Factors that are associated with an increased risk of breast cancer include:
- Being female: Women are much more likely than men are to develop breast cancer.
- Increasing age: Your risk of breast cancer increases as you age.
- A personal history of breast cancer: If you’ve had breast cancer in one breast, you have an increased risk of developing cancer in the other breast.
- A family history of breast cancer: If your mother, sister or daughter was diagnosed with breast cancer, particularly at a young age, your risk of breast cancer is increased. Still, the majority of people diagnosed with breast cancer have no family history of the disease.
- Inherited genes that increase cancer risk: Certain gene mutations that increase the risk of breast cancer can be passed from parents to children. The most common gene mutations are referred to as BRCA1 and BRCA2. These genes can greatly increase your risk of breast cancer and other cancers, but they don’t make cancer inevitable.
- Radiation exposure: If you received radiation treatments to your chest as a child or young adult, your risk of breast cancer is increased.
- Obesity: Being obese increases your risk of breast cancer.
- Beginning your period at a younger age: Beginning your period before age 12 increases your risk of breast cancer.
- Beginning menopause at an older age: If you began menopause at an older age, you’re more likely to develop breast cancer.
- Having your first child at an older age. Women who give birth to their first child after age 35 may have an increased risk of breast cancer.
- Having never been pregnant: Women who have never been pregnant have a greater risk of breast cancer than do women who have had one or more pregnancies.
- Postmenopausal hormone therapy: Women who take hormone therapy medications that combine estrogen and progesterone to treat the signs and symptoms of menopause have an increased risk of breast cancer. The risk of breast cancer decreases when women stop taking these medications.
- Drinking alcohol: Drinking alcohol increases the risk of breast cancer.
Screening
Research has proven that deaths caused by breast cancer are significantly reduced for women having screening programmes. Screening tests help to detect breast cancers early in order that the patient can undergo timely treatments, which are less invasive, have a better prognosis, and higher overall possibility of success.
A test is currently available for breast cancer: Mammography. In many countries, these are national population-based screening programs provided for people who are eligible. FV Hospital has created a year-long breast cancer screening programme based on American Cancer Society breast cancer screening guidelines
Diagnosis
Tests and procedures used to diagnose breast cancer include:
- Breast exam. Your doctor will check both of your breasts and lymph nodes in the armpit, feeling for any lumps or other abnormalities.
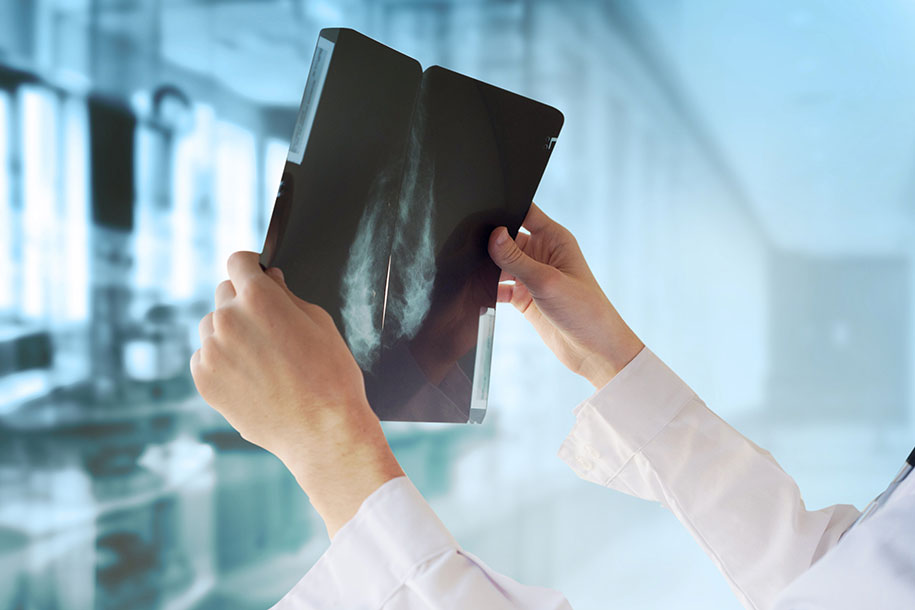
- Mammogram. A mammogram is an X-ray of the breast. Mammograms are commonly used to screen for breast cancer. If an abnormality is detected on a screening mammogram, your doctor may recommend a diagnostic mammogram to further evaluate that abnormality.
- Breast ultrasound. Ultrasound uses sound waves to produce images of structures deep within the body. Ultrasound may help distinguish between a solid mass and a fluid-filled cyst. An ultrasound is often obtained as part of the examination of a new lump.
- Breast magnetic resonance imaging (MRI). An MRI machine uses a magnet and radio waves to create pictures of the interior of your breast. Before a breast MRI, you receive an injection of dye.
- Removing a sample of breast cells for testing (biopsy). Biopsy samples are sent to Hi-Tech laboratory(*) for analysis where experts determine whether the cells are cancerous. A biopsy sample is also analyzed to determine the type of cells involved in the breast cancer, the aggressiveness (grade) of the cancer, and whether the cancer cells have hormone receptors or other receptors that may influence your treatment options.
Staging
Staging is the process of determining the size of the cancer, its location and how much it may have spread, using the tumour-node-metastasis (TNM) classification. Your cancer’s stage helps determine your prognosis and the best treatment options. We use a set of tests adjusted to each patient and each type of cancer to ensure accurate staging which is essential to decide the treatment plan.
Complete information about your cancer’s stage may not be available until after you undergo breast cancer surgery.
Tests and procedures used to stage breast cancer may include:
- Blood tests, such as a complete blood count
- Mammogram of the other breast to look for signs of cancer
- Breast MRI
- Bone scan
- Computerized tomography (CT) scan
- Positron emission tomography (PET) scan
Not all women will need all of these tests and procedures. Your doctor will select the appropriate tests based on your specific circumstances and taking into account new symptoms you may be experiencing.
Treatment
Doctors determines your breast cancer treatment options based on your type of breast cancer, its stage and grade, size, and whether the cancer cells are sensitive to hormones. Your doctor also considers your overall health and your own preferences.
Most women undergo surgery for breast cancer and also receive additional treatment before or after surgery, such as chemotherapy, hormone therapy or radiation.
At FV Hospital, all cancer cases are discussed in our weekly multi-disciplinary Oncology meeting attended by all the Hy Vong oncologists, along with radiologists and surgeons from a range of specialties. All treatments here begin with a practice called Evidence-Based Medicine. This means that our treatments are all based on international guidelines and on methods that have been proven safe and effective by the world’s leading oncologists and medical institutions.
At Hy Vong, we keep every patient and their family members informed at every stage of the treatment process and invite them to discuss their queries or concerns with our doctors at any time.
Surgery:
Operations used to treat breast cancer include:
- Removing the breast cancer (lumpectomy): During lumpectomy, which may be referred to as breast-sparing surgery, the surgeon removes the tumor and a small margin of surrounding healthy tissue. Lumpectomy is typically reserved for smaller tumours.
- Removing the entire breast (mastectomy): Mastectomy is surgery to remove all of your breast tissue. Most mastectomy procedures remove all of the breast tissue — the lobules, ducts, fatty tissue and some skin, including the nipple and areola (simple mastectomy).
- In a skin-sparing mastectomy, the skin over the breast is left intact to improve reconstruction and appearance. Depending on the location and size of the tumor, the nipple may also be spared.
- FV Hospital’s plastic surgeons can offer breast reconstruction after mastectomy.
- Removing a limited number of lymph nodes (sentinel node biopsy): To determine whether cancer has spread to your lymph nodes, your surgeon will discuss with you the role of removing the lymph nodes that are the first to receive the lymph drainage from your tumor. Sentinel node biopsy involves injecting a tracer material that helps the surgeon locate the sentinel nodes during surgery. The sentinel nodes are removed and analysed in a laboratory. If the sentinel nodes are free of cancer, then cancer isn’t likely to have spread and removing additional lymph nodes is unnecessary.
- Removing several lymph nodes (axillary lymph node dissection): If cancer is found in the sentinel node, your surgeon will discuss with you the role of removing additional lymph nodes in your armpit.
Radiation therapy
- Radiation therapy uses high-powered beams of energy, such as X-rays, to kill cancer cells. Radiation therapy is typically done using a large machine that aims the energy beams at your body (external beam radiation).
- External beam radiation is commonly used after lumpectomy for early-stage breast cancer. Doctors may also recommend radiation therapy to the chest wall after mastectomy for larger breast cancers or cancers that have spread to the lymph nodes.
- Side effects of radiation therapy include fatigue and a red, sunburn-like rash where the radiation is aimed. Breast tissue may also appear swollen or more firm. Rarely, more-serious problems may occur, such as damage to the heart or lungs or, very rarely, second cancers in the treated area.
- The process commences by defining exactly the area to be treated, the dose to be delivered and the number of radiotherapy sessions needed. At Hy Vong, we use a dedicated CT-scanner, equipped with the “LAP Laser System”, to establish the correct patient positioning for radiotherapy and to acquire the patient anatomical data. Then the tumour and organs at risk are contoured for defining their exact volumes and locations, what will allow the calculation of the correct radiation dosage and of the most appropriate radiation beams. This methodology allows us to protect surrounding tissues and healthy organs and dramatically reduces side-effects.
- Hy Vong is equipped with one of the most elaborated Treatment Planning System (Pinnacle 3D ADAC from Philips) to carry out this essential step allowing to target the tumour as effectively and safely as possible.
- This information is transferred online (avoiding thus human error) to the linear accelerator (Elekta Precise Digital Accelerator) which will deliver high-energy, dual modality radiation to the tumour.
- Healthy tissues and surrounding organs are further protected by “Low Melt Alloy Blocks” which are designed and realised specifically for each patient (basically they are physical protections), and by series of verifications using the iView GT Portal Imaging System which gives the actual image of the beam through the patient (if the patient is not positioned correctly the therapeutic radiographers will rectify the position to ensure an accurate radiation delivery).
Chemotherapy
- Chemotherapy uses drugs to destroy cancer cells. If your cancer has a high risk of returning or spreading to another part of your body, your doctor may recommend chemotherapy to decrease the chance that the cancer will recur. This is known as adjuvant systemic chemotherapy.
- Chemotherapy is sometimes given before surgery in women with larger breast tumors. The goal is to shrink a tumor to a size that makes it easier to remove with surgery.
- Chemotherapy is also used in women whose cancer has already spread to other parts of the body. Chemotherapy may be recommended to try to control the cancer and decrease any symptoms the cancer is causing.
- Chemotherapy side effects depend on the drugs you receive. Common side effects include hair loss, nausea, vomiting, fatigue and an increased risk of developing infection. Rare side effects can include premature menopause, infertility (if premenopausal), damage to the heart and kidneys, nerve damage, and, very rarely, blood cell cancer.
- All protocols used at Hy Vong are following international guidelines
- Chemotherapy can be administered orally, intravenously, or, often, via an implantable chamber. Using an implantable chamber is more convenient for the patient as they will have fewer intravenous injections, make treatments more comfortable, reduce side effects, and maximize effectiveness. This procedure is done by the anaesthesiologists of FV Hospital in a completely sterile environment.
- Chemotherapy is administered in our dedicated chemotherapy day ward, equipped with amenities such as spacious armchairs, cable television and reading materials for your comfort.
- All intra-venous infusions are prepared by a licensed pharmacist in a laminar flow sterile environment.
- The common side effects of chemotherapy include fatigue, nausea and temporary hair loss and decrease in blood cell flows, the degree of which depends on the drugs used and the drug tolerance of each individual patient. These side effects can be controlled better today than ever before.
Targeted therapy
- As researchers have learned more about the gene changes in cells that cause cancer, they have been able to develop newer drugs that specifically target these changes. These targeted drugs work differently from standard chemotherapy drugs. They often have different (and less severe) side effects.
- In about 1 in 5 patients with breast cancer, the cancer cells have too much of a growth-promoting protein known as HER2/neu (or just HER2) on their surface. Breast cancers with too much of this protein tend to grow and spread more aggressively without special treatment. A number of drugs have been developed that target this protein like Trastuzumab (Herceptin)
- Trastuzumab can be used to treat both early- and late-stage breast cancer. When used to treat early breast cancer, this drug is usually given for a year. For advanced breast cancer, treatment doesn’t stop after a year and can last a long time.
Hormone therapy
- Hormone therapy is another form of systemic therapy. It is most often used as an adjuvant therapy to help reduce the risk of the cancer coming back after surgery, but it can be used as neoadjuvant treatment, as well. It is also used to treat cancer that has come back after treatment or has spread.
- A woman’s ovaries are the main source of the hormone estrogen until menopause. After menopause, smaller amounts are still made in the body’s fat tissue, where a hormone made by the adrenal gland is converted into estrogen.
- Estrogen promotes the growth of cancers that are hormone receptor-positive. About 2 out of 3 of breast cancers are hormone receptor-positive.
- Tamoxifen blocks estrogen receptors in breast cancer cells. This stops estrogen from binding to them and telling the cells to grow and divide. For women with hormone receptor-positive invasive breast cancer, tamoxifen can be given for 5 to 10 years after surgery to lower the chances of the cancer coming back and helping patients live longer. It also lowers the risk of a new breast cancer in the other breast. For early stage breast cancer, this drug is mainly used for women who have not yet gone through menopause
- The most common side effects of these drugs include fatigue, hot flashes, vaginal dryness or discharge, and mood swings.
Follow-up care
When treatment ends, your doctors will still want to watch you closely. It is very important to go to all of your follow-up appointments. During these visits, your doctors will ask questions about any problems you may have and may do exams and lab tests or x-rays and scans to look for signs of cancer or treatment side effects.
* American Cancer Society breast cancer screening guidelines
- Yearly mammograms are recommended starting at age 40 and continuing for as long as a woman is in good health
- Clinical breast exam about every 3 years for women in their 20s and 30s and every year for women 40 and over
- Women should know how their breasts normally look and feel and report any breast change promptly to their health care provider. Breast self-exam is an option for women starting in their 20s.
- Some women – because of their family history, a genetic tendency, or certain other factors – should be screened with MRI in addition to mammogram (The number of women who fall into this category is small: less than 2%.) Talk with your doctor about your history and whether you should have additional tests at an earlier age.
(*) All biopsy samples taken at FV Hospital are sent to Hi-Tech, a state-of-the-art laboratory in Bangkok, Thailand. Hi-Tech has more than 40 top pathologists coming from the medical university, is equipped with the latest technology, and provides cutting edge immuno-histochemistry and molecular biology analysis. Reports are sent by mail within three to five days, depending on the complexity of the histopathology analysis. Molecular tests, sometimes performed to gain more information about how the tumour would respond to specific treatments, take a little longer.
For more detailed information or to make an appointment with doctors, please contact:
Hy Vong Cancer Care Centre: (08) 54 11 34 40 or (08) 54 11 33 33, Ext. 5000
Gynaecology and Obstetrics: (08) 54 11 35 35 or (08) 54 11 33 33, Ext. 6000